Combating concussions
There are a thousand ways service members can receive mild traumatic brain injuries, but basic concussion testing protocols haven’t always accounted for the intense activities required of this population. Carolina researchers have worked to change that.
The hum of engines lulls the plane’s passengers. It’s midnight, but the weight of their gear and adrenaline building in their bodies keeps them wide awake for the long morning of training exercises ahead of them. They wear green backpacks laced with yellow static lines, which unravel their T-11 parachutes as they head out into the darkness, one by one.
The summer air hits Caroline Cleveland’s face as she falls 1,250 feet toward Earth. Her chute carries her carefully but quickly. She propels toward an open field at Fort Benning and lands with a hard thud — her helmeted head smacks the turf.
“I just laid there on my back for a couple of seconds, looking up at the night sky, contemplating the cliché of why we jump out of perfectly good airplanes,” Cleveland said, chuckling.
Paratroopers in the U.S. Army make 10 to 15 jumps a year. It is a requirement of their training — and just one of many exercises that can lead to concussions. Jumps, blasts and gunfire all have the potential to damage the brain.
At the time of her jump in 2008, Cleveland didn’t consider concussions as a possible injury amidst the more visible threat of broken bones and sprained ligaments taking center stage in landing zones. She recalls being asymptomatic — but, in hindsight, she also considers herself lucky for being at low risk of getting a compounding second concussion because she had a week of downtime to rest.
Since then, the former U.S. Army captain has completed her doctorate in physical therapy at Carolina, a program she learned about while still active duty in 2013.
While researching schools, she stumbled across the faculty page of Karen “K-Mac” McCulloch, a UNC-Chapel Hill researcher studying traumatic brain injury in the military. On a whim, Cleveland sent an email to ask if she could assist in an ongoing study. Cleveland spent the next two years working with McCulloch, physical therapist Amy Cecchini and U.S. Public Health Service Capt. Henry McMillan on the project at Fort Bragg. Upon its completion, Cleveland enrolled in Carolina’s physical therapy program and continued to work with McCulloch for three more years.
“I have a different perspective today and see why screening and awareness are so important,” said Cleveland, now a physical therapist. “A concussion can be so easily overlooked in the midst of all the other things a service member is prioritizing and thinking about. They generally put their health last because they are taking care of everyone else.”
Most concussions in the military don’t happen in combat, according to McCulloch. “Concussions happen just as a result of training exercises and things that they are normally doing — things that are recreational, car crashes, that kind of thing,” she said. “And they happen more stateside than when they’re deployed.”
McCulloch began developing military specific concussion testing protocols for active-duty service members nearly 10 years ago. An expert in traumatic brain injury, she knew the current testing regimen for civilians was far removed from the rigors that military men and women often experience. Simply put, the stakes are high for returning to duty compared to, for example, an athlete who wants to return to play.
“Think about the kind of speed at which people have to react in combat zones,” she said. “If you are not at full capacity, you are potentially jeopardizing your safety and that of the people in your unit.”
A multi-task mindset
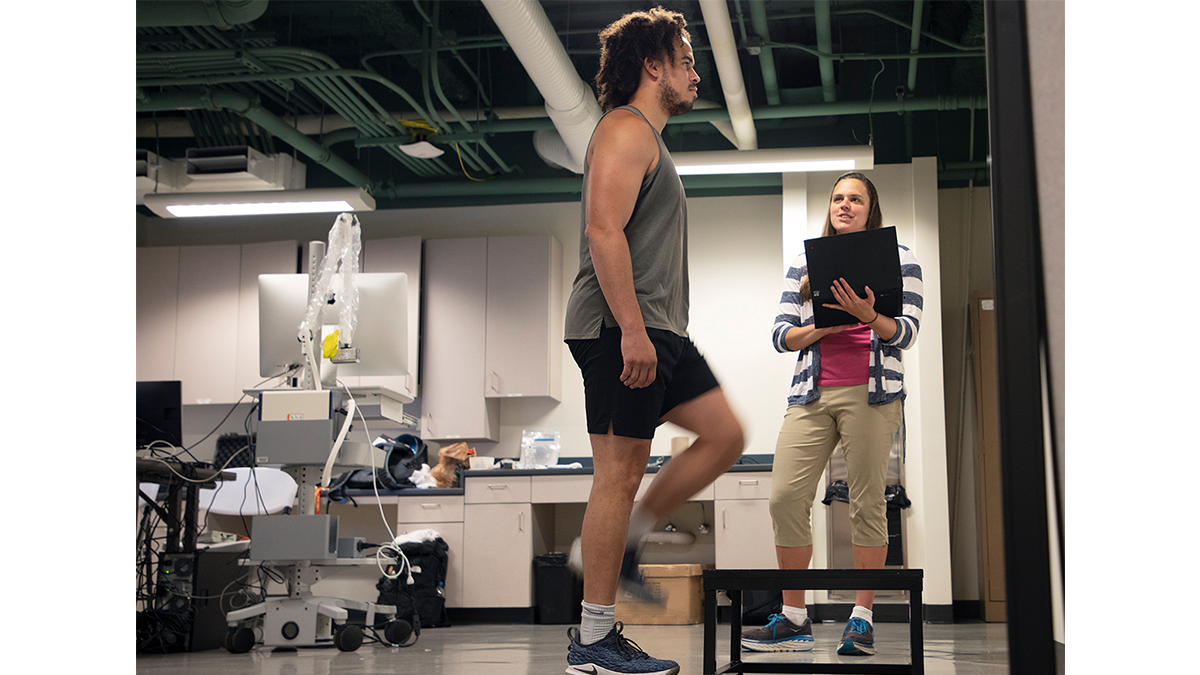
Run, roll, aim. These are the components of a combat roll, which is a standard individual movement technique used in nearly every branch of the military. Service members train to run with a weapon and complete fast, agile transitions to the ground, followed by rolls and visual targeting — all the while making smart, measured decisions. It’s a complex mix of cognitive and motor skills.
When McCulloch and a group of occupational and physical therapists began discussing concussions among this population, they took note of these rigorous requirements and observed that current testing methods only focused on singular activities. At the time, doctors tested for balance and cognition separately and then reported symptoms — the same protocol given to anyone with a potential concussion.
“When some of these people get tested, you look at them and they look fine,” McCulloch said. “They can all run. So you couldn’t just use a stopwatch and say, Yeah, that person’s too slow.It’s a lot subtler than that.”